News and Publications
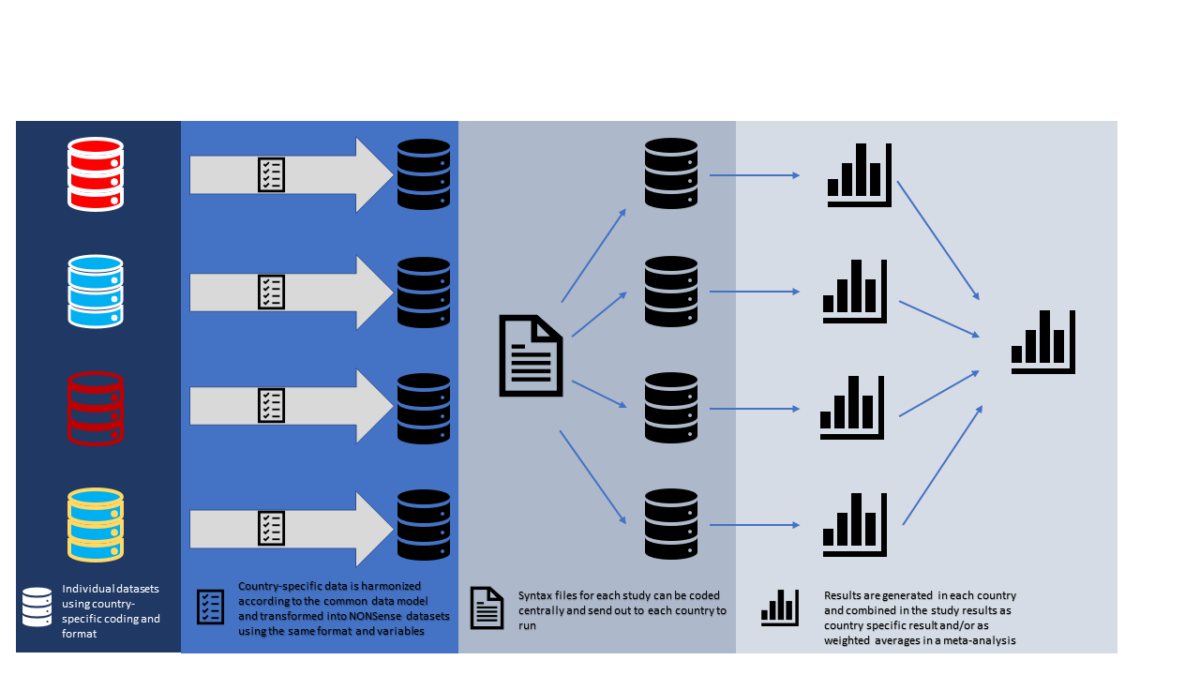
BMJ Open have published our description of our cohort and our common data model.
We published a study in Clinical Epidemiology on the use of antibiotics in children in Denmark, Finland, Norway, and Sweden.
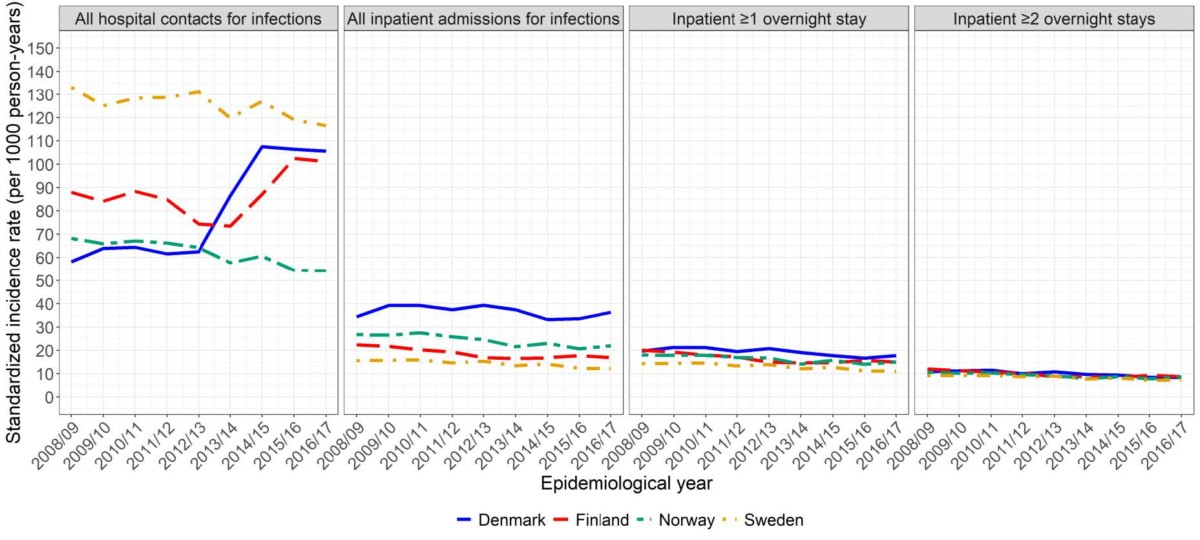
We found that the rates of all types of contacts, measured per 1 000 person-years, varied a lot between countries, from 62 in Norway to 125 in Sweden. We also found that the rates varied over time. When we only looked at hospital contacts that had resulted in overnight stays, the rates between countries were more similar.
We therefore believe that the differences in the rates of all contacts do not reflect true differences in the incidence of infectious diseases among children in the Nordic countries. Instead we think that they are a result of the differences and changes in health care organisation over time, and of coding of healthcare services for the milder diseases. The hospital contacts with overnight stays likely reflect more severe infections, which seem to be more comparable between countries and over time.
We also found that the need for hospital care was highest in early infancy followed by a second peak around 1 year of age in Denmark, Finland, and Norway. In all countries the hospitalisation rates were higher among boys compared with girls until around 5 years of age. From that age onwards, the rates were similar for both boys and girls.
These results are important because they show the trends in the number of hospitalisations for infections among children and show similarities and differences between the Nordic countries. Our study also highlights the need for researchers to carefully consider the reliability and comparability of different kinds of outcomes, like hospital contacts without overnight stays, when using data from different national health registers.
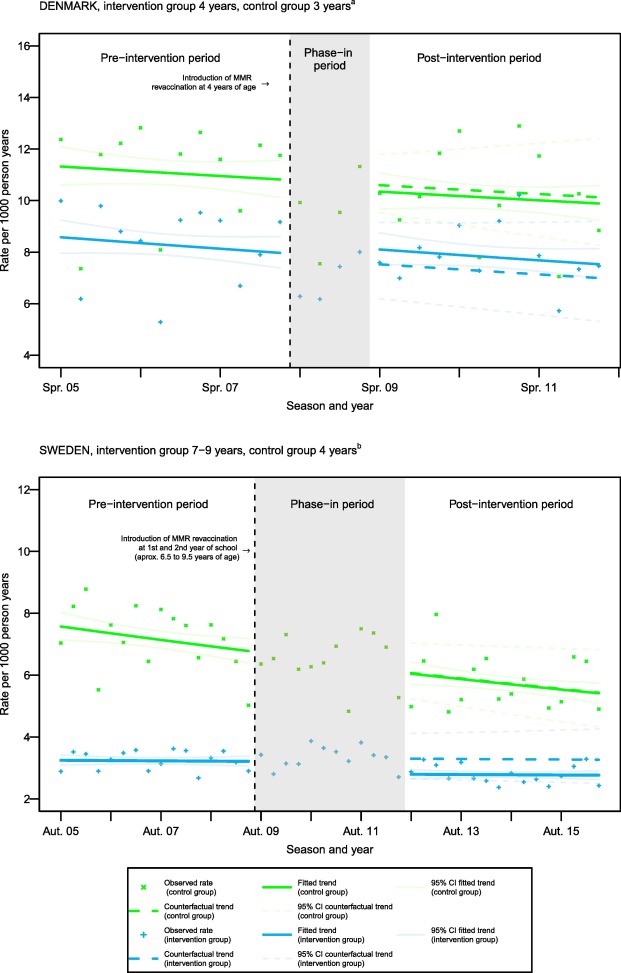
In both Denmark and Sweden, the MMR vaccine has been given in a two dose schedule for many years. The first doses is given during the second year of live, while the second dose is given later in childhood. Both Denmark and Sweden has changed the age of the second dose of the MMR vaccine (revaccination). In Denmark, the age of vaccination was changed from 12 years to 4 years in 2008. In Sweden the age was changed from 12 years to the first two school years (approximately 7 to 9 years of age) in 2007.
In this study, we used this change in vaccination program to compare the frequency of hospitalization for infections lasting 2 days or more before and after the change in the vaccination program. In Denmark, we compared the 4 year old children recommended the MMR revaccination with the 4-year old children born in earlier years who were not recommended MMR revaccination at 4 years of age. In Sweden, we compared 7-9-year old children recommended MMR revaccination with the 7-9-year old children born in earlier years who were not recommended MMR revaccination in the first two school years.
Overall, the study could not clearly confirm that recommendation for revaccination with MMR was associated with lower frequency of hospitalizations for infections lasting 2 days or more. However, relatively few number of hospitalization for infections lasting 2 days or more hampered the study and that not all children got MMR revaccination if it was part of their vaccination program.
Scientific article:
Sorup, S., Englund, H., Laake, I., Nieminen, H., Gehrt, L., Feiring, B., Trogstad, L., Roth, A. and Benn, C. S. Revaccination with measles-mumps-rubella vaccine and hospitalization for infection in Denmark and Sweden – An interrupted time-series analysis. Vaccine (in press), DOI: 10.1016/j.vaccine.2021.01.028.
